DMT and cancer
We have recently stumbled down the rabbit hole of monoamine oxidase (MAO) activity, and the potential correlation with endogenous DMT synthesis. As MAO is responsible for the rapid breakdown of DMT, it seems logical that fluctuations in MAO activity might provide a potential bio-marker for DMT formation within the body. There are two forms of MAO within the body, MAO-A and MAO-B. Both are found throughout the nervous system, MAO-A in the liver, lungs, gastrointestinal tract and placenta, and MAO-B in the blood platelets.
The plant that acts as the MAO inhibitor in the psychedelic brew Ayahuasca is Banisteriopsis caapi (B. Caapi). The active compounds in this plant responsible for the MAO inhibitions are harmine, harmaline, and tetrahydroharmine. A 2009 study published in the Journal of Ethnopharmacology found that B. Caapi suppressed MAO-A activity 2,500 times more potently than it suppressed MAO-B activity.
Another well-known plant that often accompanies DMT ingestion as a MAOI is Peganum Harmala (Syrian Rue). In a 2010 study published in the journal Food & Chemical Toxicology it was revealed that Peganum Harmala was a potent inhibitor of MAO-A activity while being a poor inhibitor of MAO-B.
This leads us to believe that one of the main indicators of DMT upregulation in the body might be MAO-A activity suppression. This is why we find it intriguing that a 2008 study in BMC Genomics revealed the following regarding MAO-A activity and cancer:
Our analysis found that significant downregulation of MAO-A, the enzyme that metabolizes serotonin, occurred in multiple tissues from humans, rodents, and fish. MAO-A expression was decreased in 95.4% of human cancer patients and 94.2% of animal cancer cases compared to the non-cancerous controls. The study proposes that low levels of MAO-A can act as a bio-marker for cancer. It was also noted that this was a significant finding based on the fact that it was a reliable change found in many different types of cancer.
Switching gears for a moment:
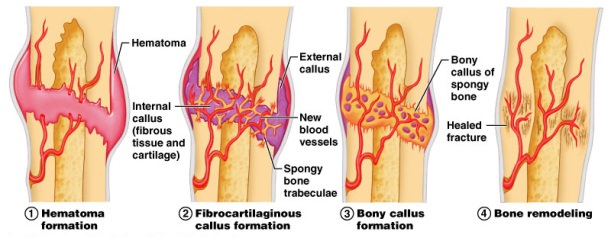
While it is clear that the body has the ability to heal itself after suffering lacerations to the skin and even broken bones if aligned properly. When it comes to disease, the prevailing medical/scientific narrative is that the body is a mistake maker. This is especially prominent when discussing any disease labeled as an autoimmune disorder, or cancer. For many decades the prevailing wisdom was that due to random, faulty genetic expression a person was susceptible to whatever debilitating conditions their fate had in store. However, in more recent times the epigenetic discussion has surged making it clear that the composition of the interior terrain of ones body such as hormone levels, autonomic signaling, ionic balance, and dominant brainwaves all contribute to genetic upregulation or downregulation.
*An excellent review of the vast number of organs/systems that can regenerate themselves was summarized in 2012 in the Journal Birth Defects Research. It almost appears as though the majority of organs in the human body can regenerate themselves to varying degrees.
An example of an epigenetic factor influencing genetic expression would be the recent 2017 study in Scientific Reports regarding the effects of 5-MeO-DMT on human mini-brains. It was observed that
out of the 6,728 identified proteins, 934 were found differentially expressed in 5-MeO-DMT-treated cerebral organoids. This signifies that biochemical exposure can change genetic signaling.
A 2011 write-up in The Journal of Physiology documents the various manners in which elevated carbon dioxide levels lead to the suppression of genes involved in the regulation of innate immunity and inflammation. A 2016 study in Pharmacogenetics and Genomics observed numerous genetic expression changes in human colon tissue associated with dietary influence. The meat-related genetic upregulation was associated with cancer, organismal injury/abnormalities, and tumor morphology.
In a 2009 study in the Journal of Biological Chemistry it was observed that over 2,600 different genes exhibited differences in expression in the pineal gland of rats based on the time of day (mid-day or midnight). That seems like a significant number of genetic expression changes in one small, single organ imagine the amount of changes found throughout the entire system!?!?
These are clear examples that genetic expression is unequivocally influenced by changes in biochemistry, diet, respiratory/metabolic fluctuations, and circadian rhythm/changes in states of consciousness. This insinuates that the random, faulty genetic expression perspective is rather incomplete and lacking. We believe the body is constantly in a state of repair. It is an infinitely complex symphony of chemicals, ions, and autonomic signaling that lead to these mechanisms transpiring. There have been many a person now and throughout history that has alleviated their incurable disease via drastic changes in lifestyle. This is not mythical or far-fetched when integrating the latest findings regarding basic biological and metabolic principles.
(When I refer to a
drastic change in lifestyle I am referring to something akin to a hamburger eating, french fry loving, soda/beer swilling, shallow breathing, sunlight shunning, stressed out insomnia transforming into a person that consumes a predominantly plant-based diet, only drinks high-quality water, receives regular daily sun exposure, practices respiratory exercises daily, and prioritizes getting 8 hours of high quality sleep every night. It would be silly for any person with a science or even non-scientific background to shun the notion that these types of radical changes would quantitatively change ones own inner terrain and subsequently their genetic expression throughout the system.)
In a chapter from the book
Recent Advances in the Biology, Therapy and Management of Melanoma, the effects of oxidative stress on melanoma development and progression were outlined. "Oxidative stress" is used to describe the harmful effects of reactive oxygen species (ROS) and free radicals including: superoxide anion radical, hydroxyl radical, and the alkoxyl radical. It was outlined in the chapter that an accumulation of ROS influenced tumor development of many different types of cancers including melanoma, leukemia, gastric, prostate, breast, and colon cancer.
As cited in the past, a 2001 study published in the journal Life Sciences observed the effects of increased hydroxyl radical generation and the effects on MAO-A and MAO-B activity. It was discovered that the generation of hydroxyl radical significantly reduced both MAO-A and MAO-B activities, exhibiting a linear correlation between both MAO-A and MAO-B activities.
This suppression of MAO activity via surges in hydroxyl radical levels points us back to the 2008 BMC Genomics study in which significant downregulation of MAO-A activity occurred in multiple tissues in various organisms that expressed different types of cancer. This would point to the potentiality for measurable DMT levels to appear in the vicinity of the greatest concentration of ROS in or around the cancer cells themselves.
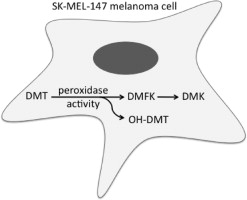
In 2014, a study published in Biochemical Pharmacology observed the biosynthesis of DMT in a melanoma (skin cancer) cell line. The researchers reported a never before seen metabolic pathway for DMT synthesis within human cells. A 2016 write-up in the journal Neura Regeneration Research cited the role of the sigma-1 receptor in terms of cellular survival in hypoxia (increased levels of ROS) and resistance against oxidative stress. The write-up also emphasized the affinity that DMT has for the sigma-1 receptor and the potential role of DMT as an anti-inflammatory agent.
What role does this compound play in terms of cancer? Does it make the disease worse or better? Perhaps DMT is much more than just a psychedelic molecule?
Earlier in this piece we cited that there are differing perspectives on the regenerative capabilities of the body. When it comes to disease, such as cancer, there are also differing perspectives. One viewpoint is that cancer occurs due to random DNA damage/mutations leading to tumor growth and eventual death. Also, the internal terrain of the body dictates biological reactions and in the case of cancer the body is attempting to sequester an overflux of detrimental components leading to tumor formation. We find it increasingly interesting that melatonin is one of the body's most powerful free radical scavengers/DNA regulators and that low levels of melatonin production has been linked to a large number of different types of cancer.
To put more succinctly, we believe that a disease such as cancer is the result of a lack of garbage men (ex. melatonin, glutathione), a chronic overflux of garbage (ex. ROS, toxic compounds) and blocked elimination pathways (ex. digestive, lympathic) that induce adaptive mechanisms. We wildly speculate that these adaptive mechanisms are our body's attempt to avoid mass cellular death and possibly poisoning of the bloodstream leading to a more accelerated death process. This might not be the popular perspective amongst mainstream, medical academics but we believe there is more than enough supportive data to warrant this viewpoint.
We believe that one of DMT's role in cancer is to provide a protective mechanism to the body by attempting to neutralize the elevated levels of ROS within cancer cells in order to slow down proliferation. Future studies are necessary in order to verify the role of DMT in cancer.
There are numerous abnormal ionic/electrical based qualities associated with cancer cells such as a more depolarized cell membrane potential, a hyperpolarized mitochondria, elevated intracellular sodium concentrations, and suppressed intracellular chloride concentrations.
In 2013, a case study report published in SAGE Open Medicine would review 9 separate cases of people reporting the effects of Ayahuasca ingestion on different types of cancer (prostate, brain, ovarian, uterine, stomach, breast, and colon cancers). Seven cases were reported as improvements, one was considered a regression, and one was too difficult to evaluate. The author would propose a theoretical model regarding the mechanisms of how the effects transpired as follows:
DMT binds sigma-1 receptors with moderate affinity and, at high concentrations, is also capable of inhibiting voltage-gated sodium channels. Thus, DMT may exert two types of effects through sigma-1 receptors: at low concentrations, it regulates calcium flow from the endoplasmic reticulum to the mitochondria, whereas at higher concentrations, it exerts diverse effects at the plasma membrane region. The effect on calcium influx into the mitochondria may be extremely important for cancer treatment given that an energetic imbalance between excessive cytosolic aerobic glycolysis and reduced mitochondrial oxidative phosphorylation (the Warburg effect) was recently suggested as the seventh hallmark of cancer. This metabolic profile of cancer cells is accompanied by a hyperpolarization of the mitochondrial membrane potential that may be reduced by the calcium influx triggered by DMT binding to the sigma-1 receptor at the mitochondria-associated endoplasmic reticulum membrane. This effect may facilitate the electrochemical processes at the electron transport chain inside the mitochondria, thus increasing the production of reactive oxygen species (ROS) and leading these cells to apoptotic pathways. When high DMT concentrations induce sigma-1 receptor translocation to the plasma membrane, many cellular effects would occur due to the receptor's interaction with different ion channels. At high concentrations of DMT, a calcium influx and mitochondrial membrane depolarization might be enough to also activate the permeability transition pore (PTP), inducing mitochondria swelling, rupture, and apoptosis.
It is important to note that in the write-up many of the 7 subjects who recovered from cancer were also noted to integrate a plant-based diet into their habits. Obviously this could play an additional factor in their systemic recovery process.
The discussion of Ayahuasca and it's therapeutic efficacy regarding cancer is an interesting one as there have been many anecdotal cases of remission of disease following ingestion of the psychedelic brew. Some are reported to be more spontaneous in nature while others have been cited to take months of consistent ingestion. There are numerous studies showcasing various cancers coinciding with dysfunction of autonomic nervous system signaling (1, 2, 3, 4, 5). While the cellular mechanisms correlating with remission will be difficult to verify, we do believe that the neuroplasticity inducing properties of Ayahuasca correlate with alterations (a fix of sorts) in the signaling between the brain and the autonomic nervous system. A recent 2017 write-up in New Scientist addresses nervous system signal dysfunction and the potential therapeutic effects of blocking nerve signaling to cancer cells in an attempt to thwart disease progression. It is interesting to note the effects of synthetic analgesics cited in the write-up being that the endogenous molecule 5-MEO-DMT has been shown to have analgesic properties as well.
In regards to our own perspective of the mechanisms for the effectiveness of Ayahuasca, there lies the potentiality that the reversal of faulty signaling coincides with region specific release of DMT (amongst other biochemicals) in the cancer site that induces cancer remission via a rebalancing of the ionic composition of the cell via sigma-1 receptor activation. While this is highly speculative if this were to be the case, it might insinuate that DMT has the potential to be synthesized in glial cells found abundantly throughout the central nervous system (we suspect DMT is synthesized in the same places that melatonin is synthesized glial cells included). We don't believe that it's a case of DMT release from the pineal finding its way to the tumor site.
While the cancer-DMT discussion is ultimately very complex and involves many layers of the body, it seems important to discuss when speculating on the mechanisms for healing. Spontaneous remission is a scientifically and medically accepted term for
unexplainable disappearance of disease within the body. It's a basic concession that something occurs without understanding the mechanisms for its occurrence. In many cases of spontaneous remission, the subjects claim a spiritual phenomena that occurs alongside the healing mechanism. We've come across many anecdotal claims of this type of healing from Ayahuasca, yoga/meditation, Wim Hof Method, hypnosis, Ajna Light exposure, deep visualization exercises, and even placebo. Interestingly enough these are all altered states of consciousness that we have speculated to correlate with increased DMT levels. We've also touched upon the measurably altered electrical activity in the brain and body during these states as well.
Hopefully more studies can be developed going forward to better understand our endogenous healing mechanisms and DMT's role within it. However, an acceptance of a distinct change in perspective of physiology might be necessary to better understand what is actually taking place. We believe that DMT has a much more common and functional role in the body other than solely mystical experiences.
PS. In some small percentage of cases, a person is born with a congenital disease that manifests due to numerous factors. We need to remain cognizant that even a fetus can be exposed to detrimental environmental factors via the placenta that will ultimately effect their gene expression and formation of disease. However, there are cases of people (a small percentage) suffering from a rare disease for unknown reasons which can be traced back to a gene but that doesn't necessarily equate to blaming genetics for all disease formation.
http://q4lt.com/cancer-and-dmt